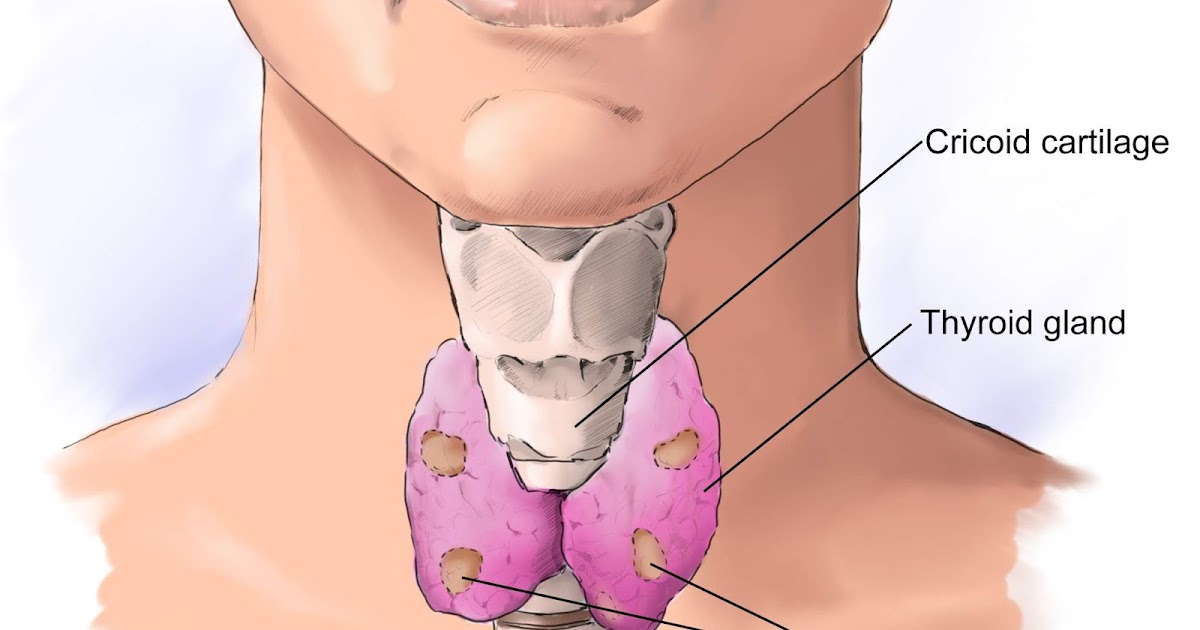
Thyroid nodules in children
Increasingly, nodules of the thyroid gland in children began to be detected, especially with the introduction of an ultrasound of the thyroid gland with a medical examination before school.
A thyroid nodule is an area of its tissue that differs from the rest of the thyroid tissue during ultrasound (usually more than 5 mm in size) or on palpation (feeling).
So, the nodes of the thyroid

gland in children can be:
not tumors
– Colloidal node (nodes)
– Pseudo-nodes of Hashimoto’s thyroiditis
– Hyperplasia of thyroid follicles up to 5 mm
– Ectopic thymus (up to 9 years old)
– Cysts
– Subacute thyroiditis
tumors:
benign – adenoma
malignant:
a) differentiated cancer: papillary, follicular
b) undifferentiated (anaplastic)
c) medullary cancer.
But according to the picture of the ultrasound, it is sometimes difficult to determine what kind of node it is. Therefore, for nodes larger than 1 cm, it is accepted to carry out TAB. TAB stands for Fine Needle Aspiration Puncture Biopsy. The method of diagnosing nodules located relatively close to the surface of the body is carried out under the control of ultrasound.
With nodes less than 1 cm, indications for TAB in children are:
signs of malignancy by ultrasound
family history of cancer
history of head and neck irradiation.
The reliability of TAB 98% is a very high indicator for a diagnostic method.
Depending on the results of the biopsy of the node, further management tactics are carried out (observation, medical or surgical treatment of the node (s). The results of the biopsy are evaluated according to the BETHESDA SYSTEM 2010 system, and have 6 post-biopsy cytological conclusions.
When observing thyroid nodules in children, an increase in the size of a nodule is not always a risk of malignancy, but a sign that “the child grows – the nodule is also growing.”
When a node is detected, it is advisable to control the level of thyroid hormones: TSH, free T4, and in case of signs of AIT (autoimmune thyroiditis) – the level of antibodies to TPO and TG.
For nodes more than 1 cm – determination of calcitonin and parathyroid hormone, especially with a family history of malignant thyroid masses.
Thyroid dysfunction: hypothyroidism or hyperthyroidism with thyroid nodules in children is rare, more often the nodes are accompanied by a normal hormonal background.
Iodine deficiency is not the main reason for the appearance of thyroid nodules in children in St. Petersburg and the Leningrad region, and therefore there is no direct indication for their treatment with iodine preparations (iodomarin, etc.).
Hormones (L-thyroxine https://en.wikipedia.org/wiki/Levothyroxine, etc.) are prescribed for thyroid nodules – in combination with nodules with reduced thyroid function (hypothyroidism), this is without surgical intervention. Indications for hormone therapy after surgery are determined by the volume of surgery performed and the histological conclusion of the removed material, in a replacement or suppressive dose.