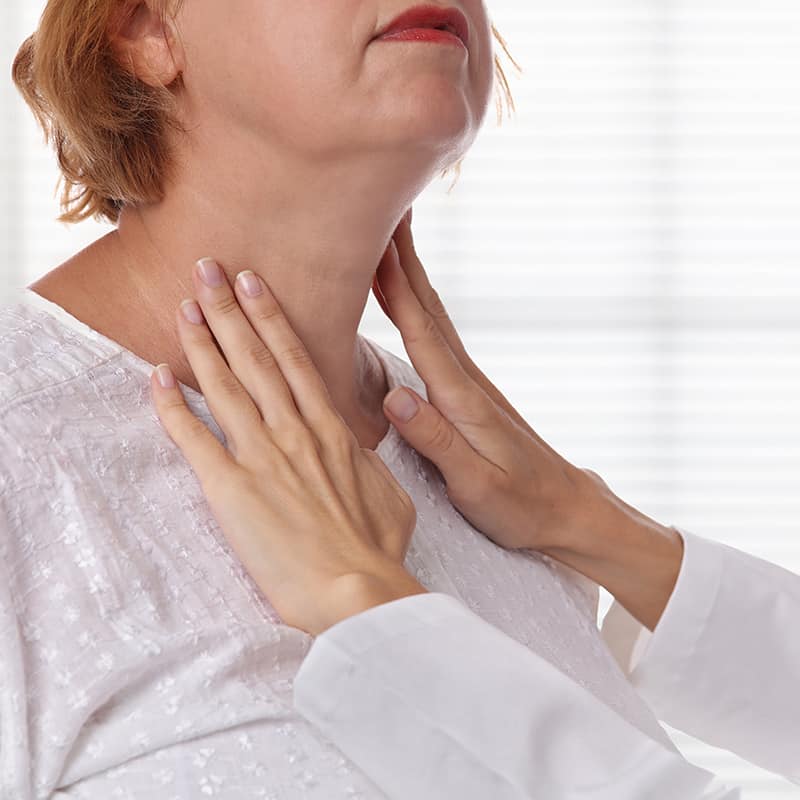
Autoimmune thyroiditis. “Mystery of the Century”. Part 1
Autoimmune thyroiditis has become a mystery not only in the 20th, but now in the 21st century. Until now, the reasons causing it have not been solved, there are many theories – there are no definitive answers. Although the theory of environmental pollution is more likely!, But today is not about that. In relation to this diagnosis, a certain “blurring” has appeared, it is given to everyone who needs it and who does not need it, and they are often treated quite lightly.
But this is a serious autoimmune inflammatory process in the thyroid gland, which cannot be predicted, its course cannot be predicted! A sharp turn during AIT can occur at any time. Today I will tell you about it that you have never read, the source of information is very reliable, clinical observations of the disease began in the late 60s of the 20th century.
So,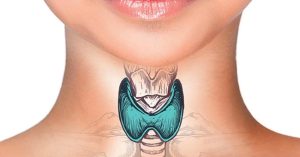
AIT does not always debut with a chronic process, it can begin acutely and have a picture completely similar to the picture of subacute thyroiditis, the treatment in this case will be the same.
Or another option is possible: during a sluggish AIT, an acute period may occur and it will also be completely similar to subacute thyroiditis. The only thing that can distinguish AIT from subacute thyroiditis is the density of the thyroid gland, which can reach the characteristics characteristic of Riedel’s goiter (the thyroid gland with AIT is often very dense, which does not happen with adjusting thyroiditis), that is, the density of thyroid tissue can reach (+++ +).
Yes, there is such a classification of thyroid density (0 / + / ++ / +++ / ++++). Moreover, it is interesting that in previous years it was customary to treat the acute course of AIT with goiter with a combination of Prednisolone and T3 (in doses of at least 25 μg), without T4, because, as a rule, acute AIT is accompanied by a pronounced goiter (a sharp increase in the thyroid gland), which is well fed treatment with T3 (which is an active hormone, not a prohormone like T4).
AIT began to often be combined with DTG (diffuse toxic goiter), and DTG against the background of AIT flows easier and remission can occur faster than without AIT.
DTZ goes into AIT easily, but the transition of AIT to DTZ is extremely rare. Although I had such patients, and in one of them, the transition from AIT to DTZ occurred in the 3rd trimester of pregnancy, which was previously considered generally incredible. I’m talking about the unpredictability of the flow of AIT.
AIT proceeds more easily in iodine-deficient regions of Russia, but in regions with a normal iodine content, it can worsen its course. And therefore, Russian comrades 🙂 who moved to Italy, Spain, the USA and other hot countries for permanent residence need to be on their guard, many have already brought from there a sharply developed AIT with dysfunction, hypothyroidism and high TSH levels.
A low titer of antibodies in AIT is not a “good process”: cry:, it is just a different type of immune response: high antibodies in AIT are a humoral type of immunity, and a low titer is a cellular one, it is not yet known which is better. With the humoral type, patients respond more easily to iodine and preparations with it (it is better tolerated) than with the cellular type, with the humoral type, anti-hepatitis drugs, vaccines and other immunity stimulants are “not good”.
If you are “lucky” and the immune reactions during AIT are not uncontrolled, then AIT will have a latent course with intact thyroid function and will not require lifelong administration of L-thyroxine preparations.
When compensating for hypothyroidism against the background of AIT, given the absence of T3 in pharmacies, T4 euthyroidism can be achieved easily, but T3 euthyroidism is not, why with T4 monotherapy signs of hypothyroidism may persist (this may be a consequence of uncompensated T3 hypothyroidism), it is fashionable to draw an analogy here with the concept of T4 – / T3-thyrotoxicosis. T3 thyrotoxicosis is treated harder and slower.
Rather sad news: the younger AIT 18+ started, the harder it will be (this does not apply to children, they have their own characteristics, only adults), although there are exceptions to this rule – I have had patients who, after a long the course of AIT entered spontaneous remission and went away even with high doses of HRT with 100 μg of L-thyroxine – in 0 μg! I warned – the course of AIT cannot be predicted !!
Considering the above information, it should be noted: only an endocrinologist, not a gynecologist, not a general practitioner should deal with AIT treatment – this is a disease with great “nuances and details”!
AIT can really provoke the development of hypertension, and its treatment (AIT) can improve the course of hypertension or stop it altogether.
AIT can be combined with any thyroid diseases: cancer, nodular non-toxic and toxic goiter, etc. How these diseases in combination affect each other is still studied.
Already in the 80s of the 20th century, it was mentioned in the scientific literature – intolerance to L-thyroxine in patients with AIT, which is not recognized by many doctors, unfortunately, and even by endocrinologists. But in fact, there is a small percentage of people with developed intolerance to L-thyroxine preparations or intolerance to L-thyroxine in doses over 25 mcg. I observed at least 10 people with such a reaction, the most striking example was a 70-year-old man (Novgorod region), after surgery for retinoblastoma of the orbit (this is a complex tumor process of the eye tissue), he developed hypothyroidism with TSH 40 mIU / ml and with an attempt to prescribe thyroid hormone drugs to him – his blood pressure dropped sharply, dizziness and nausea began, he could not get up, when he missed taking the drug L-thyroxine, it became easier for him and it was decided not to continue the treatment, and was interpreted as an abnormal reaction to L- thyroxine, an increase in TSH – was interpreted as a “compensation reaction”, since during hypothyroidism metabolic processes in the body slow down – therefore, tumor metastases will develop and progress more slowly !!!
The nodes (colloidal) accompanying AIT are not always a pseudo-nodular (pseudo-nodular) form of AIT (for AIT, false nodes are often characteristic – that is, not a “tissue growth”, but an inflammatory process – lymphoid infiltration without the phenomenon of “tissue plus”. These nodes can be both nodular goiter and toxic adenoma and cancer, parathyoma (formation of the parathyroid glands), and even lymphoma and any other process, therefore, in many cases, a biopsy of thyroid masses is indicated !!!!! AIT and almost the main one in the diagnosis of AIT !! while all other methods – ultrasound, hormones (blood), scintigraphy, iodine uptake curve – are non-specific methods and make the diagnosis probable!
There are concepts of abortive form of AIT and spontaneous remission of AIT. It sounds happy 🙂 The abortive form of AIT is a variant of “self-recovery” when no signs of AIT remain over time! Occurs, rarely, usually 10 or more years after the onset of AIT (I’ve seen such options).
Remission of AIT can also be spontaneous after long-term drug therapy (for example, complete cessation of L-thyrxine intake, while maintaining a small titer of antibodies to the thyroid gland). What makes this pathology even more mysterious.
Conclusions: AIT can have a primary chronic course, or with an acute onset or frequent exacerbations, with and without dysfunction of the thyroid gland, hypothyroidism or, more rarely, hyperthyroidism.
AIT https://en.wikipedia.org/wiki/Autoimmune_thyroiditis with an abortive course or remission, or with transformation into another pathology – DTZ, etc., AIT can be expressed as a hypertrophic form (a sharp increase in the thyroid gland) or an atrophic form (a sharp decrease in the thyroid gland), with an increase (humoral type of immunity) or without an increase in titer thyroid antibodies (cellular type) immunity, less often – mixed type of immunity …. against the background of either iodine deficiency or without deficiency. iodine, now ALL THIS must be treated somehow … To be continued in the second part …